Inflammatory Acne: What Red, Swollen Breakouts Mean
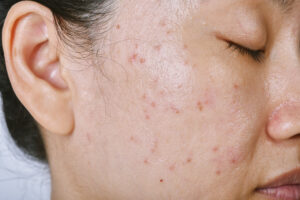 If your acne looks angry, feels sore, and takes forever to heal, there’s a good chance you’re dealing with inflammatory acne. These breakouts tend to be red, swollen, tender, and stubborn, and they often don’t respond to the usual drugstore solutions. Instead of fading in a few days, they linger, flare repeatedly, and may leave marks behind long after they’re gone.
If your acne looks angry, feels sore, and takes forever to heal, there’s a good chance you’re dealing with inflammatory acne. These breakouts tend to be red, swollen, tender, and stubborn, and they often don’t respond to the usual drugstore solutions. Instead of fading in a few days, they linger, flare repeatedly, and may leave marks behind long after they’re gone.
Inflammatory acne can be frustrating, painful, and confusing, especially if you feel like you’re “doing everything right.” Understanding what inflammatory acne is, why it behaves differently, and how it should be treated can help you take a more effective (and less aggravating) approach to clearing your skin.
What Is Inflammatory Acne?
Inflammatory acne develops when a clogged pore becomes irritated or infected, triggering an immune response within the skin. That immune reaction is what causes the redness, swelling, warmth, and discomfort that set inflammatory acne apart from milder forms of acne.
Unlike blackheads and whiteheads, which sit closer to the surface, inflammatory acne forms deeper within the skin. Because of this, breakouts often feel sore to the touch, may not come to a head, and take longer to resolve.
Common types of inflammatory acne include:
- Papules: red, inflamed bumps without visible pus
- Pustules: red bumps with a white or yellow center
- Nodules: large, firm, painful lumps beneath the skin
- Cysts: deep, pus-filled lesions with a higher risk of scarring
These breakouts are more likely to leave dark spots or scars if not treated properly, especially when inflammation is ongoing.
Inflammatory vs. Non-Inflammatory Acne
One of the most important distinctions in acne treatment is whether acne is inflammatory or non-inflammatory.
Non-inflammatory acne includes blackheads and whiteheads. These develop when pores become clogged with oil and dead skin cells but don’t trigger much redness or swelling. They’re often easier to manage with topical treatments like retinoids or salicylic acid.
Inflammatory acne involves more than just clogged pores. Bacteria, excess oil, and an overactive immune response all contribute to visible inflammation. This is why treatments that simply dry out the skin often make inflammatory acne worse rather than better.
Understanding this difference matters because using the wrong approach can prolong breakouts, increase irritation, and raise the risk of scarring.
What Causes Inflammatory Acne?
Inflammatory acne causes are usually multifactorial, meaning several factors work together rather than a single trigger being responsible.
Excess Oil Production
When sebaceous glands produce too much oil, pores clog more easily. Trapped oil creates an environment where bacteria can thrive, setting the stage for inflammation.
Acne-Causing Bacteria
Cutibacterium acnes naturally lives on the skin, but when it becomes trapped inside a clogged pore, it can multiply. In some people, this triggers a strong inflammatory response that leads to redness, swelling, and tenderness.
Hormonal Fluctuations
Hormones (particularly androgens) stimulate oil production. This is why inflammatory acne commonly flares during puberty, around menstrual cycles, during pregnancy, or later in adulthood.
Immune System Sensitivity
Not everyone’s immune system reacts the same way to clogged pores and bacteria. Some people have a heightened inflammatory response, which can make breakouts larger, redder, and more painful.
Friction, Sweat, and Irritation
Tight clothing, helmets, backpacks, masks, and frequent sweating can trap heat and moisture against the skin. This irritation can worsen inflammation, especially on the jawline, chest, shoulders, and back.
Why Inflammatory Acne Often Hurts
Inflammatory acne forms deeper in the skin than surface-level breakouts. As swelling builds inside the pore, pressure increases around nearby tissue and nerve endings. This pressure is what makes nodules and cysts feel sore or painful, even if they never form a visible head.
Trying to pop or squeeze inflammatory acne usually makes things worse. It can push bacteria deeper into the skin, intensify inflammation, and significantly increase the likelihood of scarring.
How to Treat Inflammatory Acne
Treating inflammatory acne requires a thoughtful approach that reduces bacteria, regulates oil production, and calms inflammation without damaging the skin barrier.
Topical Treatments
Dermatology-guided topical treatments may include:
- Prescription retinoids to prevent clogged pores
- Benzoyl peroxide to reduce acne-causing bacteria
- Topical antibiotics when appropriate
- Anti-inflammatory ingredients to help calm redness
Consistency matters, and using too many active products at once can increase irritation.
Oral Medications
For moderate to severe inflammatory acne, oral acne medications may be recommended, such as:
- Oral antibiotics to reduce bacteria and inflammation
- Hormonal therapies for hormonally driven breakouts
- Isotretinoin for severe, scarring, or treatment-resistant acne
A dermatology provider can help determine which options are appropriate based on acne type, severity, and medical history.
Anti-Inflammatory Acne Treatment Strategies
Anti-inflammatory treatment for acne focuses on calming the skin rather than stripping it. This often includes:
- Gentle, non-foaming cleansers
- Non-comedogenic moisturizers to support the skin barrier
- Avoiding harsh scrubs and over-exfoliation
- Simplifying routines to reduce irritation
Supporting the skin barrier is especially important when treating inflammatory acne.
In-Office Treatments
Certain in-office treatments can help reduce inflammation and speed healing, including:
- Cortisone injections for large, painful cysts
- Chemical peels formulated for acne-prone skin
- Laser acne treatment or light-based therapies in select cases
How to Get Rid of Inflammatory Acne Safely
If you’re searching for how to get rid of inflammatory acne, patience is key. These breakouts don’t disappear overnight, and overly aggressive treatments often prolong healing.
A safer, more effective approach usually involves:
- Following a treatment plan designed for your specific acne type
- Giving treatments adequate time to work
- Avoiding picking or squeezing breakouts
- Addressing underlying triggers such as hormones or friction
Progress may be gradual, but consistent care can significantly improve results over time.
When to Seek Professional Care
Inflammatory acne should be evaluated by a dermatology provider if:
- Breakouts are deep, painful, or persistent
- Acne leaves dark marks or acne scars
- Over-the-counter treatments aren’t effective
- Acne is affecting confidence or daily life
Early treatment can help control inflammation and reduce the risk of long-term skin damage.
Expert Care for Inflammatory Acne
If red, swollen acne isn’t improving on its own, expert care can help. Dermatologists and dermatology providers at Schweiger Dermatology Group offer personalized treatment options designed to manage inflammatory acne and reduce the risk of scarring. Call 844-DERM-DOC or book online today to schedule an appointment.

